The ever-changing climate for dentistry during the COVID-19 makes reopening plans a challenge for practice owners.
Read on for the latest, in-depth information – plus find details of free support at the end of the guide - from Global Dental Managing Director Ryan Devenish.
Contents:
1, Surgery sanitising: The challenge, electrostatic technology, X-mist, Biofilm, reassuring practice users.
2, Essential infrastructure upgrades: A sneeze screen mistake to avoid, choosing the right option, an essential recommendation, some vital protection questions to consider.
3, Handwashing solutions: Guidelines, recommendation.
4, Staying safe at work: HEPA...the evidence, an important methodology, suction systems in the Coronavirus era, the big question.
Updated 16/07/20: The latest CDO letter to dentists, and its first 24th July deadline, means decisions around Coronavirus measures are now unavoidable with the main focus for dentists falling on how to manage government guidelines with the least possible financial impact. Find our response to the letter, and some brief recommendations, here.
Preparing to Reopen a Practice – Your Questions Answered
1, Surgery Sanitising
How to clean pathogens from hard to access places? What methods exist to sanitise contact points like door handles to best reassure clients and colleagues? How to remove biofilm from dental chairs?
Ryan explains...
The surgery sanitising challenge: "How do you intend to ensure you can safely disinfect every plastic, laminate, Corian, metal and material surface within your surgery?
"As we’re learning from initial studies this Covid-19 virus can survive on any surface for a number of hours or even days. This study published in the New England Journal of Medicine on 17th of March suggests that the virus can last at least 72 hours on plastic, 48 hours on stainless-steel, 24 hours on cardboard and four hours on copper surfaces.
"Added to this, the fact that - according to the study - the virus can remain viable in aerosols for three hours is going to make effectively disinfecting surfaces within a dental surgery challenging.
"From my experience of visiting many dental practices and surgeries over the years work surfaces within a surgery tend to have significant number of items on them and would be difficult to wipe down effectively. Take a dental treatment centre for example, the various angles and intricacies of the unit mean there are many surfaces and areas that are going to be difficult to effectively wipe.
"Regular touch points such as handles, computer keypads, delivery unit and light handles are the obvious ones that can disinfected by a wipe or spray. However what about the work surface around smaller equipment that hasn’t been moved for while: the amalgamator?"
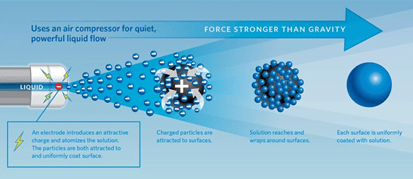 Using electrostatic technology: "This is one reason why we’ve been considering the technology of electrostatic sanitising as a method of helping manage the disinfection of multiple surfaces in dental surgeries. As the applicator emits the fog it charges the particles with a negative charge and, as the vast majority of surfaces are neutral, the fog is attracted to the surface.
Using electrostatic technology: "This is one reason why we’ve been considering the technology of electrostatic sanitising as a method of helping manage the disinfection of multiple surfaces in dental surgeries. As the applicator emits the fog it charges the particles with a negative charge and, as the vast majority of surfaces are neutral, the fog is attracted to the surface.
"When the negative particles are emitted the fact they are the same polarity means they repel each other creating an even mist, and subsequently they attracted to the opposite polarity in the surfaces meaning that the particles reach many areas that cannot be accessed by standard cleaning methods.
"The next question is how to apply this technology effectively and cost sensitively within a dental practice? There have been some studies indicating that the virus can survive in some circumstances for a lot longer periods so perhaps a weekly fogging of the premises via an engineer would be a suitable solution. This could probably be achieved for around £80 a week for a full practice on an annual contract basis.
"On the other hand, the practice should purchase a machine circa £1,500 plus the disinfectant and carry out the procedure themselves every evening to maximise the process and really provide a very safe environment for their staff."
X-Mist and dental surgeries: "Another item we’ve been looking into is the X-mist product and how that could potentially be used as a extra safety net for sanitising surfaces.
"It is the nature of the dental surgery having a lot of difficult surfaces, with materials and equipment on worksurfaces, intricate elevations and areas of equipment that has made us consider these misting solutions.
"The X-mist is quite a simple, cost effective and ingenious method of simply fumigating a room that may have been used for AGP’s or potentially had in a Covid-19 positive patient."
Biofilm: "Biofilm is definitely nothing new for the dental industry. Biofilm itself, and removing it with various treatments, has been the source of many a blocked tube or valve within a dental treatment centre. But, let’s be honest, this is likely to be brought into relief in a fresh way over this current crisis. That's why we have recently started recommending the Belmont water treatment products: B100 Chair Upholstery Cleaner, B300 Surface Disinfector, B500 DUWL Intro Kit, B700 DUWL Daily Maintenance and B900 Periodic Shock Test.
"The big question around Biofilm? With so much of our equipment being sat with very little action have we dropped our vigilance in testing and treatments?
“For all practice owners current doing more study and reading, this is a good time to ensure you’re up to speed on this irritating yet important topic. A great link to start with can be found here.
Reassuring practice users: “I’ve been encouraging practices that are taking steps like this to talk about it on their communications with their staff and patients and take the time to exhibit to them that they’re really serious about their safety.”
Surgery sanitising summary: Consider all available technologies to sanitise hard to reach areas and challenging surfaces plus don't forget to communication with practice users.
More Questions? For free advice simply
 or call
or call
 .
.
Plus find details of free support at the end of this guide
2, Essential Infrastructure Upgrades
 NHS guidelines call for ‘sneeze screens’ in place for two years. But how to make these aesthetically appealing? Which materials are most effective? And do waiting room booths etc need to be protected?
NHS guidelines call for ‘sneeze screens’ in place for two years. But how to make these aesthetically appealing? Which materials are most effective? And do waiting room booths etc need to be protected?
Ryan explains...
Sneeze screens...a mistake to avoid: "Sneeze screens…what a name! But these are important measures to take and where more important than for a receptionist who might meet 100 different patients in a single day.
"The risk of a cough a sneeze or even just speech aerosols reaching and enveloping the receptions staff is real.
"The market for these in the general industrial community has exploded, making Perspex not dissimilar in price to glass. However what intrigues me is what level or size of screen is really appropriate in the dental setting.
"You can purchase 800 x 800 flat sections of Perspex which sit on the desk top meaning that you end up peering through it like through a cloudy pair of cheap plastic glasses. I believe they probably do the job to a point but I am slightly sceptical that it will provide much protection.
"The other aspect to consider is how significant is the risk of them toppling over if bumped by a patient. Could they fall on a receptionist?"
Choosing the right sneeze screen: "Something fixed is safer and more effective. Cost is of course a factor to consider again but there are some reports from within the NHS facilities teams have been told to ensure their screens are strong enough to last for 2 years at a minimum so spread over this length of time, and with a lot of suppliers offering payment plans, it doesn’t seem as big of a factor if you’re wanting to maintain the practices’ exquisite look and feel.
"An important issue to consider: the aesthetics of a dental practice, and especially in the reception and public areas, are increasingly important as this is where first impressions are gleaned. Will it make a patient think “wow, this team care about how I feel when I visit” and “what a lovely practice, and how clean and well maintained it looks, this feels safe”.
"To this end we have been investigating and now have a good solution for the installation of proper glass screens, that both look impressive, and serve an excellent purpose.
"Having the advantage over Perspex that they don’t scratch, are clear and are fixed so no risk of falling. Glass screens are surely, therefore. the way forward for aesthetically conscious and conscientious practice owners wanting to protect their staff.
Sneeze screen fitting...an essential recommendation: “You may think sneeze screens will need drilling of your expensive reception desk.
"A system exists - simply ask me for more information - whereby the fitter can, by installing a false top, not mark the existing desk at all. So in a couple of years when this advice is relaxed they can be removed and with a bit of filler and paint for the ceiling/walls with no trace. On the other if you chose to retain it for the long haul to protect staff, glass lasts….and doesn’t deteriorate."
Some vital protection questions: "There are so many other aspects to protective screening and social distancing that could impact how practices run..here’s a few thought provoking questions:
- Should practices be creating more smaller waiting areas to reduce crowding.?
- Will more surgeries be required to achieve UDA targets, with gaps between patients?
- Should we be creating 'waiting booths' for families with dividers between seating groups?
- Can we install hand washing facilities in the waiting rooms
"I’ll continue to update this guide or publish information to cover these points”
Essential infrastructure upgrades summary: Carefully weigh up the material and fitting method used for sneeze screens and take time to consider
Need help? For no obligation support
 or call
or call
 .
.
Plus find details of free support at the end of this guide
3, Handwashing Solutions
Encouraging handwashing at your practice entrance needs an effective, efficient, secure and attractive contactless solution. Which units would perform best for your practice? Can units be branded to match a practice interior?
Ryan explains...
Handwashing guidelines: "We all know and have been told that handwashing is the way forward for the long haul, after all Point 2 of the government guidelines states:
- Wash your hands often using soap and water, and dry them thoroughly.
- Where available, use sanitiser outside your home, especially as you enter a building and after you have had contact with surfaces.
- Avoid touching your face.
Handwashing recommendation: "Sanitiser and handwashing are both going to become a feature of practice waiting rooms. My recommendation: make them slightly more aesthetically pleasing by procuring some branded dispensing stations.
"In addition: consider an auto handwashing station, after all even hand gel is not as good as properly washing your hands."
Handwashing solutions summary: Consider the importance of ensuring every practice visitor washes their hands properly and explore the available options for branded and auto handwashing stations.
More Questions? For free advice simply
 or call
or call
 .
.
Plus find details of free support at the end of this guide
4, Staying Safe at Work
 What role can a HEPA 14 Air Purifier play in removing airborne pathogens? Which PPE items will needed going forward?
What role can a HEPA 14 Air Purifier play in removing airborne pathogens? Which PPE items will needed going forward?Safe dental procedures and HEPA filters: "With aerosol-generating procedures, previously the everyday norm, now banned other than in theatre-like conditions, there are a lot of unanswered questions around the management of aerosols and air quality in general.
"There are many air purifiers on the market ranging hugely in cost and complexity and it’s really not conclusive whether any of them are going to make a huge impact.
"One key question I am wrestling with: if you re filtering air that has potentially contaminated aerosols carried within it, then doesn’t the filter just become a hotbed and breeding ground for the virus?
"I don’t believe HEPA can be decontaminated therefore they remain until they are disposed of, and in future where in use should be treated as highly contagious waste. This is not to mention the unit itself, it is actively dragging all particles within the air towards itself and all surfaces of the unit is more at risk of becoming contaminated with viral load.
HEPA...the evidence: "The British Orthodontic Society state in their document 'PPE and Decontamination for Aerosol Generating Procedures in Orthodontics (AGPs)': "High-efficiency particulate air (HEPA) is an efficiency standard of air filter. European standards dictate that a HEPA filter must remove at least 99.95% of particles whose diameter is equal to 0.3 μm. The diameter of droplet (>5 μm) and aerosol (<5μm) thought to be important in the spread of COVID-191 fall within the diameter of that captured by a HEPA filter. The evidence behind the use of HEPA filters in a healthcare setting is inconclusive, but it is thought to help prevent infection in a hospital setting where they are employed in theatres and isolation rooms. It has been hypothesised that air filtration could be employed to reduce the severity and spread of COVID-1915 . There is no evidence to support or refute their use to prevent transmission of COVID-19 in a dental setting. As such, they may play a role in the decontamination of Clinical and non-Clinical areas during the current pandemic. If air filtration with a HEPA filter is being considered for use in a non-clinical environment, the size and efficiency of any unit should be tailored to the size of the room it is used in."
"Further to this, doesn’t an air purifier in the corner of the room effectively draw the aerosol across the room from the patients, potentially drawing them past the clinician and staff? Which brings us onto the idea of intraoral suction products.
"There is, again, a batch of various machines springing up across the market place but do they really achieve the desired outcome? Yes they may draw aerosols away from the clinician directly but do they, like the purifiers, become a hotbed of virus infection that creates as significant health hazard for the staff member dealing with it?
An important methodology: "As far as I can see the only somewhat proven methodology at the moment is the basic principal of air changes, so ventilation of practices is going to become increasingly important.
"From experience, historically it is an area of capital investment within a practice that is difficult to justify and see the benefits of, however that has just been significantly raised in its importance I would imagine.
"The Public Health England’s guidelines for "Reducing the risk of transmission of COVID-19 in the hospital setting” states that: "Clearance of infectious particles after an AGP is dependent on the mechanical/natural ventilation and ACH within the room. A single air change is estimated to remove 63% of airborne contaminants; after five air changes, less than 1% of airborne contamination is thought to remain. In an isolation room with 10 to 12 ACH a minimum of 20 minutes is considered pragmatic; in a side room with 6 ACH this would be approximately one hour. Advice should be sought from the local IPCT.”
“To me this escalates the need for mechanical ventilation, and if practices need to be seeing more than one patient an hour is there going to need to be some rethinking of the infrastructure of a practice.
"There are ways in which this can be implemented in a cost-effective manner, and anyone with ceiling voids in their various rooms will be a lot better placed to have this installed. However even for those that don’t there are ways of making it not too aesthetically bruising on the eye."
Suction systems in the Coronavirus-era: "There is another significant factor in all of this as dentists have for many years had a powerful suction system installed and indeed they use it for the majority of procedures.
"So I would suggest that now is the time to review your suction, get it tested to check its effectiveness and maybe someone somewhere will do some studies into a more advanced aspirator end piece to catch a more significant volume of the aerosols created. Perhaps the most cost effective step would be to utilise a funnel connected to the high-volume aspiration hose.
"There is however a caveat with this and that is that these suction units don’t have any functionality for filtering or disinfecting the air that it removes from the patients mouth and surrounding areas. This is a really important thing for the dentist to assess.
"Should you be moving your suction pump outside somewhere? Its a serious consideration as not only does it remove the air from the building but it removes the noise and potential leaks and spills also.
"Is it definitely vented best it can be to outside? Small extraction fans can be placed in the back of cupboards and small ducting can be installed into some pretty slim areas to get the fumes outside with a bacterial filter installed."
Safe working...the big question: "All in all there is a lot of uncertainty around what is required to get dentistry working again: does it need expensive and complex equipment, is the benefit worthy of the investment? Or perhaps the question is 'what is the most effective investment I can make'?
It goes without saying that SOP for PPE is going to be different from pre-Covid times. In the case of Urgent Care Centres the latest SOP guidelines can be found here.
Updated 03/06/20: The latest return to work document from the British Dental Association is now online here while the Faculty of General Dental Practitioners document can be accessed here.
Updated 05/06/20: A just-released SOP document from the Chief Dental Officer includes one section some practice may find to be a lifeline.
Some headline takeaways…
- The importance of equipment checks.
- The value of a screen to protect reception colleagues.
- Ventilation – a key update as a room with negative pressure will only need a 20mins wait between patients vs one hour for neutral pressure.
- Clarity around PPE.
- Guidance on high-speed suction.
We can help dentists respond to the new SOP in two ways:
-Suction equipment, ventilation and reception: We will carry out an on-site suction check of all aspiration points free of charge in any practice north of Coventry to continue to support UK dentistry. We will also advise on ventilation and ‘sneeze screen’ options.
-PPE in stock for rapid dispatch: Our latest stock of PPE, including PPF2 masks, will always be shown in our online shop. PPE items are locally held and ready for immediate shipping.
More Questions? For free advice simply
 or call
or call
 .
.
Announcing: Our Free Practice Reopening Advice Line
We’ve been calling dentists to ask how we can help and even offer a listening ear. We also offer the same support, and much more, to every UK practice.
To access our complimentary Practice Reopening Advice Service
 for an immediate response or call
for an immediate response or call
 .
.
If Global Dental can help, he’ll explain how and if on-site work falls outside Global Dental’s area he'll help find the right support. At no charge and with no obligation.
Ps – Why are we doing this? Earlier in the COVID-19 crisis we announced a package of support for UK dentists including: free engineer support calls for any dentist, free help to source in-demand PPE, ongoing Coronavirus-response information publishing.
In short: we want to support UK dentists back to work. Tell us how we can help.
Global Dental
Environments | Support | Equipment since 1996






.png?width=700&name=GD%20blog%20image%20CV%20(3).png)
 WhatsApp Support:
WhatsApp Support: